Yes, many women notice hip or joint pain as they enter midlife. Hormone changes during menopause can lower estrogen and affect bone strength, tendon tissues, and joint lubrication¹.
These shifts in hormone levels can make the hips feel sore or stiff. While every woman’s experience is different, menopause and hip joint pain are often connected. Understanding this link helps women know that the pain is real and manageable with the right steps.
At SensIQ, we help women face menopause with confidence and clear information. Created by neurologists, SensIQ offers science-based guidance to support the body and mind. Dr. Luke Barr, Chief Medical Officer, explains that knowing how menopause affects the body helps women stay mobile and feel their best.
Key Takeaways
- Menopause can lead to hip and joint discomfort because lower estrogen and changing hormone levels affect bones, tendons, and joint lubrication.
- Women experience symptoms such as stiffness, aching, and reduced flexibility, often worsening at night or after long periods of sitting.
- Early attention to these symptoms helps identify conditions such as gluteal tendinopathy or bursitis before they limit mobility or comfort.
- Physical therapy, regular physical activity, and good posture can support joint health and help reduce pain naturally over time.
- Supplements that support joint health may be useful as part of a wellness plan, but results vary, and medical guidance is always recommended.
What Causes Hip and Joint Pain During Menopause?
Hormonal Changes, Estrogen Loss, and Cortisol Imbalance
When estrogen levels drop, collagen production also decreases². This can cause joints and connective tissues to become less flexible. Lower estrogen and rising cortisol (a stress hormone) can also slow recovery after physical activity.
These changes in hormone levels explain why menopause can lead to hip and joint discomfort. Gentle movement, stress control, and rest can all help the body adapt.
How Menopause Affects Tendons, Muscles, and Joints
Estrogen helps protect tendon tissues and the fluid-filled sacs that cushion joints. With reduced hormone levels, these areas may dry out and lose elasticity, resulting in friction and discomfort.
Less circulation and weaker muscles may also lead to pain in menopause, especially in the hips and knees. Staying active with walking or stretching supports joint health and flexibility.
Gluteal Tendinopathy and Other Related Conditions
Menopause-related hip pain can come from gluteal tendinopathy, which happens when the tendons near the hip become irritated or inflamed over time.
As estrogen levels decline, tendon tissue loses some of its strength and elasticity, increasing the risk of strain during daily activities such as walking or climbing stairs. This condition often causes a deep ache on the outer side of the hip that worsens when lying on that side or standing for extended periods.
Bursitis, another common source of discomfort, occurs when the fluid-filled sacs that cushion the joints become sensitive or swollen. Early signs of arthritis may include stiffness or limited range of motion, especially in the morning.
Dr. Luke Barr explains that recognizing these changes early allows healthcare providers to recommend physical therapy, strengthening exercises, and posture adjustments that support joint comfort and mobility while helping women stay active safely.
What Does Menopause Hip Pain Feel Like?
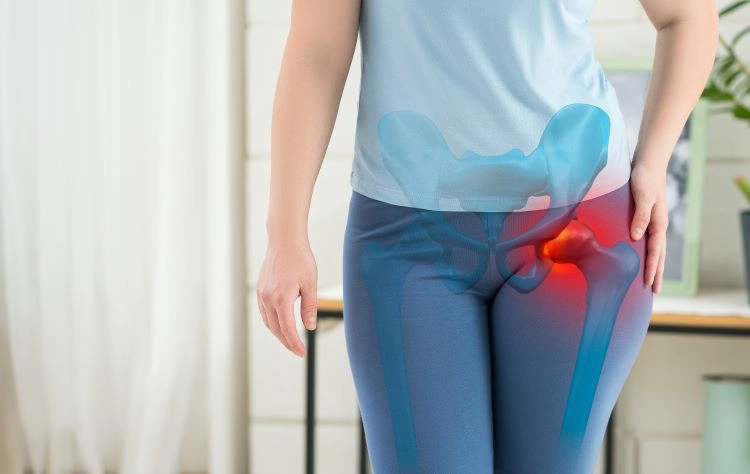
Typical Sensations and Discomfort Patterns
Menopause and hip joint pain may manifest as dull aching or sharp discomfort, particularly when walking, standing, or lying on one side.
Some women experience stiffness after sitting for a long time, but it often improves with gentle movement. These symptoms show how hormone changes may reduce joint lubrication and flexibility. The pain can also spread to nearby muscles, causing the lower body to become tense.
Nighttime Hip Pain and Lower Back Stiffness
Hip pain in menopause often gets worse at night. A cooler body temperature and slower circulation can make joints stiffer. The lower back may also feel tight if core muscles weaken. Using supportive pillows, moving during the day, and keeping a steady sleep schedule may ease these symptoms.
When Pain Suggests a Different Condition
Sometimes joint pain during menopause has other causes. A doctor should check for pain with swelling, redness, or limited movement. These signs may indicate arthritis, nerve compression, or low bone density. Getting an early diagnosis helps guide safe ways to reduce pain and improve movement.
How Doctors Diagnose Hip Pain in Midlife Women
What Is a Red Flag for Hip Pain?
Red flags include sudden swelling, bruising, or pain that makes walking hard. These may indicate a fracture, infection, or a serious joint issue. Women with these symptoms should see a doctor right away. A clinician can tell if menopause and hip joint pain are connected or if something else is causing it.
Tests and Imaging to Find the Cause
To find the cause of hip pain during menopause, doctors may perform physical exams, order blood tests, or perform imaging such as X-rays or MRIs. These help separate hormonal changes from structural problems.
Dr. Luke Barr says that a good diagnosis leads to clear wellness plans with exercise, physical therapy, and lifestyle steps to protect joint health.
How to Relieve and Prevent Hip Pain During Menopause

Effective Menopause Hip Pain Exercises
Physical activity is one of the best ways to manage menopause-related hip pain. Simple moves like yoga, swimming, or cycling can keep muscles strong and joints flexible. Explore our menopause exercise plan for more low-impact routines that support joint health.
Regular physical activity also supports circulation and may help in reducing inflammation. A physical therapist can build a safe plan to strengthen the hips and relieve pain.
Safe Medications and When to Use Them
Over-the-counter pain relievers such as acetaminophen or NSAIDs may help with mild joint pain³. Always follow a doctor’s advice before using them. Supplements that support joint health may also support overall wellness, but results may vary*.
Dr. Luke Barr advises women to check with a healthcare professional before adding any supplement to make sure it fits their needs.
Physical Therapy, Strength, and Lifestyle Habits for Long-Term Relief
Physical therapy supports joint movement and flexibility. It builds muscle strength around the hips and improves balance. Therapists can show posture or stretching exercises that may ease everyday musculoskeletal pain. Combining therapy with hydration, balanced meals, and enough rest supports healthy joints over time.
Tracking Recovery and Protecting Joint Mobility
Tracking symptoms helps women understand what affects their pain. Writing down activities and comfort levels can reveal patterns, such as excessive sitting or stress.
Maintaining a healthy weight, managing hot flashes with cooling habits, and choosing foods that may help in reducing inflammation all support joint comfort. Over time, consistent care helps women feel more mobile and confident staying active.
Common Questions About Menopause and Hip Pain
Can menopause affect mobility or walking?
Yes. Reduced estrogen and lower muscle mass can affect balance and coordination. Many women experience mild unsteadiness or joint stiffness when hormone levels change. Regular stretching, balance training, and low-impact exercise can help maintain mobility and support joint health.
Does inflammation cause menopause-related hip pain?
It can contribute. Hormone shifts may make tissues around the hips more sensitive, leading to mild inflammation or soreness. A balanced diet, stress management, and physical therapy help reduce inflammation naturally and support overall comfort.
Why does hip pain feel worse at night during menopause?
At night, the body’s circulation slows and hormone levels shift slightly, which may increase stiffness and sensitivity. Lying in one position for too long can also put pressure on sore joints. Using a body pillow or changing sleeping positions can reduce discomfort and improve rest.
Can menopause lead to hip arthritis or long-term joint problems?
Menopause can lead to changes that affect joint tissues, but not every woman develops arthritis. Lower estrogen levels may influence bone and cartilage health over time. Staying active, supporting bone strength through nutrition, and addressing pain early with a healthcare provider can help protect joint function.
When should women seek medical help for hip pain?
See a doctor if hip pain is severe, sudden, or lasts more than a few weeks. Swelling, redness, or trouble walking are also signs to get checked. A professional can determine whether menopause and hip joint pain are related or whether another condition needs attention.
References
- Hinge Health. (2025, February 10). Menopause and hip pain: Causes, treatments, and exercises for relief. https://www.hingehealth.com/resources/articles/menopause-hip-pain/
- Mehta, P. (n.d.). Menopause hip pain. Resilience Orthopedics. https://www.resilienceorthopedics.com/hip/menopause-hip-pain/
- Chidi-Ogbolu, N., & Baar, K. (2019). Effect of estrogen on musculoskeletal performance and injury risk. Frontiers in Physiology, 9, 1834. https://doi.org/10.3389/fphys.2018.01834
*These statements have not been evaluated by the Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease.

