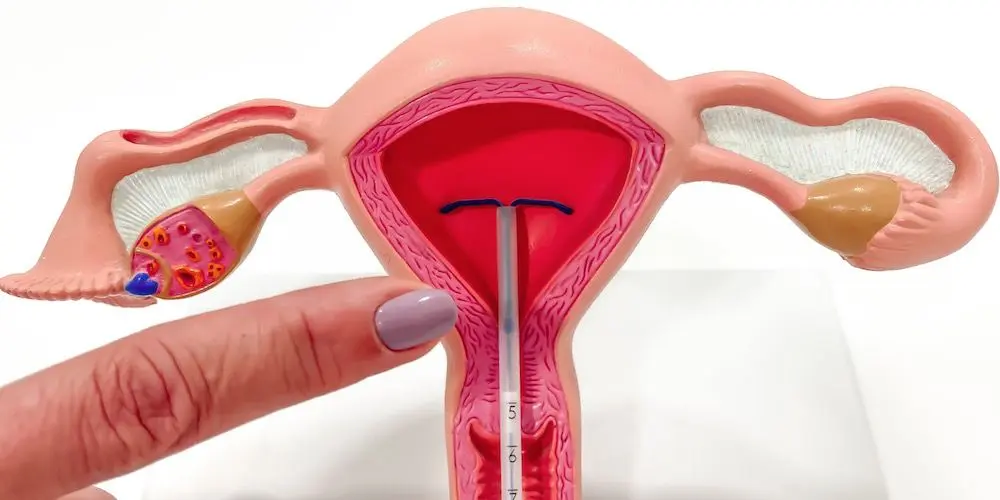
An intrauterine device, or IUD, can be a helpful option during perimenopause because it supports contraception while also addressing some symptoms like heavy periods and irregular bleeding.
The benefits of an IUD for perimenopause include reduced menstrual flow, protection of the uterine lining, and convenience as a long-term birth control method. Risks may involve side effects such as cramping, spotting, or changes in hormone levels, depending on the type chosen.
Guidance from a healthcare provider is essential to determine whether a copper or hormonal IUD is most suitable. Overall, an IUD offers a safe and effective choice for women navigating the transition between perimenopause and menopause.
At SensIQ, we recognize that the changes of perimenopause can affect not only your body but also your daily confidence and clarity. This article explores IUD for perimenopause, explaining how it works, its benefits, potential side effects, and how to discuss options with your doctor.
Guided by the clinical expertise of Dr. Luke Barr, Chief Medical Officer at SensIQ, our goal is to provide evidence-based insights to help women make informed decisions about their health.
Key Takeaways
- An IUD for perimenopause may help manage heavy bleeding, irregular periods, and provide reliable long-term contraception.
- Hormonal IUDs, such as Mirena, release progestin that supports the uterine lining and may reduce heavy periods, while copper IUDs offer a hormone-free birth control option.
- Some women may experience side effects like cramping, spotting, or irregular bleeding, which often improve within a few months.
- An IUD can usually stay in place through the transition from perimenopause to menopause, though doctors often recommend removal about one year after the final period.
- Women should consult their healthcare provider to decide which type of IUD is most appropriate and to discuss alternatives such as hormone replacement therapy or non-hormonal birth control methods.
What Happens in Perimenopause
Perimenopause is the stage before menopause. It often starts in the late 30s or early 40s. At this time, hormone levels change and may cause hot flashes in your 30s, night sweats, and irregular periods. These changes can be confusing, especially for women who still want to prevent pregnancy.
Should women in perimenopause consider an IUD?
Yes, an IUD can help many women in perimenopause. It is a safe and reliable birth control method. It may also help manage heavy periods and irregular bleeding. For women who want to avoid hormone replacement therapy (HRT), an IUD is a simple option that works with the menstrual cycle.
How an IUD Helps in Perimenopause
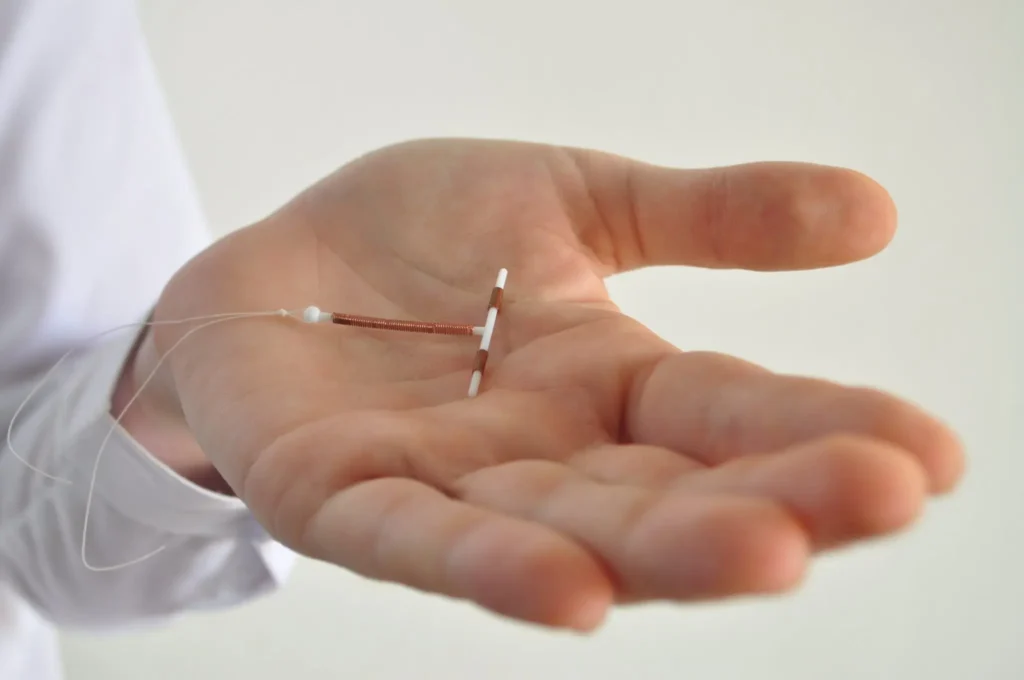
IUD for perimenopause symptoms
An IUD may ease symptoms linked to the menstrual cycle. Hormonal IUDs release progestin, which helps keep the uterine lining thin and can reduce heavy bleeding. By supporting stability in the lining of the uterus, an IUD may make cycles easier to manage.
IUD for perimenopause bleeding
Many women in perimenopause have heavy periods. An IUD may help reduce bleeding by thinning the uterine lining¹. This can support daily comfort and lessen the burden of heavy periods.
IUD and weight gain in perimenopause
Weight gain in perimenopause is common. It is often due to age, lifestyle, and hormone levels. Some women think IUDs cause weight gain, but most studies show no consistent link². Weight changes are more likely from perimenopause itself, not from the device.
Types of IUDs and Their Role
Best IUD for perimenopause
The best IUD for perimenopause depends on individual needs. Hormonal IUDs may help reduce heavy bleeding, while copper IUDs are effective for women who want a non-hormonal birth control method. Both provide strong protection against pregnancy.
Hormonal IUD for perimenopause
Hormonal IUDs release a small amount of progestin into the uterus. This may help with irregular bleeding and support a healthy uterine lining³. Doctors often suggest this option for women with heavy periods or irregular bleeding.
Mirena IUD for perimenopause
Mirena for perimenopause is a well-studied option. It is FDA-approved for birth control and management of heavy periods. Research suggests that Mirena may help thin the lining of the uterus, which can make irregular bleeding easier to manage.
Does Mirena lower estrogen levels?
No. Mirena works by releasing progestin into the uterus. It does not lower estrogen levels. Women still make their own estrogen, which is why symptoms like hot flashes and night sweats may still occur.
Non-hormonal IUD for perimenopause
Copper IUDs do not contain hormones. They prevent pregnancy by stopping sperm from reaching the egg. They may suit women who cannot or do not want hormones. However, some may notice heavier bleeding or more cramps.
Benefits and Side Effects

Benefits of an IUD for perimenopause
- Strong and long-term birth control method.
- May reduce heavy periods and irregular bleeding.
- Supports the health of the uterine lining.
- Easy to use – no daily steps needed.
Side effects of IUD in perimenopause
Some women may have cramps, spotting, or irregular bleeding after insertion. Side effects often improve within a few months. Copper IUDs may make periods heavier, while hormonal IUDs often make them lighter. Understanding these differences helps women choose the most appropriate option.
IUDs and the Menopause Transition
Transitioning from Perimenopause to Menopause with an IUD
An IUD can often stay in place as women move from perimenopause to menopause. It continues to prevent pregnancy during this stage, which is important since ovulation can still happen until menopause is complete.
Most doctors suggest keeping the device for one year after the final menstrual period to ensure full protection. At that point, it can usually be removed unless there is another medical reason to keep it.
How to Recognize Menopause While Using an IUD
Because an IUD may reduce or even stop bleeding, it can be difficult to know when menopause has started. In these cases, doctors may run hormone level tests or rely on other common symptoms such as hot flashes, night sweats, or changes in mood and sleep.
These signs can help confirm that menopause has begun, even without obvious menstrual changes.
Alternatives to IUDs
How IUDs compare to hormone therapy
Medical Guidance
Who is a good candidate?
Good candidates include women with heavy bleeding, irregular periods, or those who need reliable birth control. Suitability depends on health history and personal needs.
Questions to ask your doctor
- Should I choose a hormonal or copper IUD?
- How long can I keep the IUD during perimenopause and menopause?
- What side effects should I expect?
When to seek medical advice
See a doctor if you have severe pelvic pain, unusual discharge, or sudden changes in bleeding. These could be signs of complications.
FAQs about IUDs and perimenopause
Can an IUD cause hot flashes?
No, these come from hormone changes, not the IUD.
Does an IUD affect fertility long-term?
Fertility usually returns once the IUD is removed.
Can an IUD prevent endometrial cancer?
Some research suggests hormonal IUDs may support a healthy uterine lining³, but results vary and more studies are needed.
References
- Bayer HealthCare Pharmaceuticals Inc. (2022, August). Mirena (levonorgestrel-releasing intrauterine system) [Prescribing information]. U.S. Food and Drug Administration. https://www.accessdata.fda.gov/drugsatfda_docs/label/2022/021225s043lbl.pdf
- National Institute for Health and Care Excellence. (2021, May 24). Heavy menstrual bleeding: Assessment and management (NG88). https://www.nice.org.uk/guidance/ng88
- Committee on Practice Bulletins—Gynecology, & Long-Acting Reversible Contraception Work Group. (2017). Practice Bulletin No. 186: Long-acting reversible contraception: Implants and intrauterine devices. Obstetrics & Gynecology, 130(5), e251–e269. https://doi.org/10.1097/AOG.0000000000002400